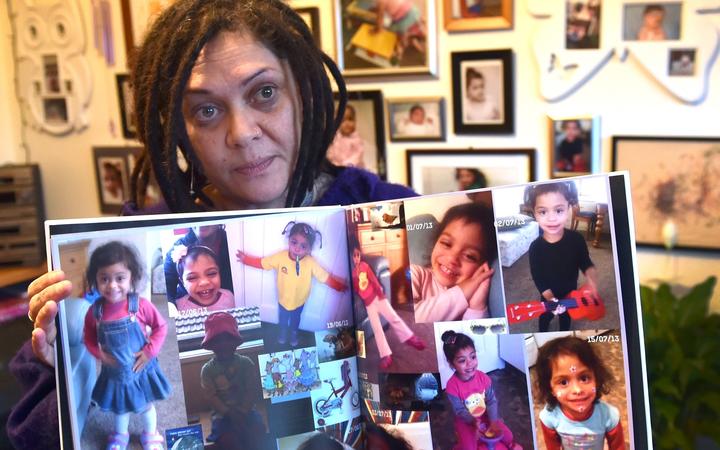Practice
Supporting informed consent
It can be easier said than done regarding the right to give informed consent.
This right is particularly prominent in members’ policies covering Privacy, Child Protection and access to health treatment. It is supported by the policy requirement for people to be given information in understandable ways.
But how do we ensure that people understand the information we provide or the form we ask them to sign? There will always be variables. The language, abilities, age and maturity of people we are working with will affect if and how information is understood. So will the nature and type of information and situation in which it is given.
But there are some general steps we can take to assist people to understand the information we give them or want them to know.
Steps to support understanding
Plain language – Use plain and simple language and break down complexity. Avoid jargon and technical terms that can make it difficult for the average person to understand.
Translation – Offer and arrange for interpreters as necessary for verbal interactions; provide a translated version of the agreement, form or other information into the person’s primary language and ensure the translation is accurate.
Make it visual – Use aids such as diagrams, pictures, charts, or illustrations can help convey complex concepts. These can often make it easier for individuals to grasp the content.
Encourage and answer questions – invite questions, answer and provide further clarification as needed.
Allow time – people often need time to digest information gradually, discuss it with others and time to come back to you to discuss.
Documentation Offer a copy of the written form or agreement to the person in advance so that they can review it at their own pace and come prepared with questions.
Accessibility Support Sse accessible formats and make provisions for Braille, large print, and digital text for screen readers, if necessary.
Simplify – For complex information or if an agreement or form contains intricate or lengthy clausesbreak them down into simpler parts, explain each part separately and check understanding as you go.
Make it real – Offer real-life examples or scenarios to help make the information real and to show what it might mean in practice. In this way, abstract concepts become much more tangible.
Proving Informed Consent
As a members of the Policy Place online service, most of you are subject to external audits and checks. It is therefore important that you document – the steps taken with people to assist their understanding of terms, information, agreement and to properly support them to make informed decisions.
There are many other aspects to the Informed Consent policy that need to be evidenced in individual files. But being able to show that staff are taking the steps needed to ensure people’s understanding oof information, forms etc is an important start.
Policy tips for cultural responsiveness
It’s foundational
Cultural responsiveness is foundational for any social service, health or other agency in Aotearoa/New Zealand. It’s a core requirement of the new Health and Disability Standards, which take effect on 28 February 2022. It’s also central to the Social Sector Accreditation Standards.
The foundational nature of cultural responsiveness should reflect across an organisation’s policies and procedures for operations, governance, programmes, client services etc. It begins with an understanding and acknowledgment of the history of Aotearoa and Te Tiriti o Waitangi.
At the Policy Place, we reflect “foundational” in our online policy and procedure service by having a group of integrity policies that speak to the heart of the agency – policies addressing Te Tiriti o Waitangi, Equality and inclusion, the Kaupapa of the agency, Disability Confidence, Whānau Engagement and Pasifika. Because the policies are part of an online platform, they are meant to, and can easily, be considered as part of other policy requirements in areas like HR and operations.
It’s a big concept
In the health sector, cultural responsiveness involves a broad meaning of “culture.” It includes, but is not limited to, values, attitudes and beliefs that can be associated with ethnicity, age, gender identity, sexuality, socioeconomic status, occupation, iwi affiliation, religion, spirituality and disability.
Responsiveness means having regard to culture and involves self and organisationally -aware practice. Those providing a service have undergone a process of reflection of their own cultural identity and the impact this has on policies, practice and services.
This is not just the job of one policy. At the Policy Place we have policies addressing person- and whānau-centred practice so that the circumstances, needs and values of those served trump preset programmes.
Power dynamics must be recognised and challenged
A criterion of the Ngā Paerewa Health and Disability Standard is that it is safe to ask in the organisation ‘how is institutional and systemic racism acting here?”
Policies should encourage and support staff and leadership to identify and do something about systemic inequalities, for example:
- that access by those traditionally underserved by the social and health sectors will be monitored and prioritised in planning;
- identify and address the impacts of colonisation (eg monocultural workforce, policies and practices) eg strengthen and build your Māori workforce; outreach strategies).
Develop a plan with your policy
At the Policy Place, cultural responsiveness policy is supplemented by a Cultural Competency and Responsiveness plan. In this way, online members get the benefits of policy as well as a plan that they can use and modify to fit their circumstances and aspirations.
If you’re not part of our online service, you can implement your own policy with a plan. Your policy can state the important and enduring requirements. Your plan can support you to action them. With your team, identify your responsiveness goals, key actions you will take to achieve them, how you’ll know you’re progressing and review dates.
How we can help
Cultural responsiveness is embedded in the suite of online policies and procedures we provide to our members. Our members come from all walks of life so our challenge is to make cultural responsiveness policies appropriate and meaningful for different contexts.
It’s an ongoing project of improvement that we’re committed to.
If you want help with your policies and procedures, contact us.
Helpful Resources
For some great resources on cultural responsiveness check out these:
Ministry of Health, Te Tiriti o Waitangi (Te Tiriti) Framework
Ministry of Health, Te Tiriti o Waitangi (Te Tiriti) Framework
Inclusive Health Principles and Strategies
Intellectual Disabilities ODI Guidance and resources for employers and business owners
Learning and education modules on understanding bias in health care
3 tips for your Use of Restraint policy
The new Health and Disability Standards come into effect in February 2022. At the Policy Place we’re updating our online policies for our members. We’ve just finished updating the Use of Restraint policy.
If your policies are due for an update to come into line with the new Health and Disability standards then now is a good time to join the Policy Place online policy and procedure service. Contact us now to find out more.
But if you’re into DIY here are some tips on what to cover in your Use of Restraint policy.
The goal is elimination
Your policy purpose should clearly state upfront your agency’s intent to eliminate or at least, minimise the use of restraint against any client.
The purpose should reflect throughout your policy and procedure. Importantly, require that restraint be used only as a last resort and only after alternatives like de-escalation have been tried.
Assessment and planning are important
If a person is identified during assessment to have challenging behaviours that may necessitate the use of restraint, this should be addressed in planning with that person and their family, whānau, other supports.
In this context, everyone can come to a common understanding and agreement about relevant behavioural triggers, what works, doesn’t work, relevant cultural values and how, when and what should be applied to address challenging behaviour if prevention and de-escalation don’t work.
Accountability is crucial
The recent release of the Abuse in Care interim report in Aotearoa/NZ highlights the importance of accountability for the use of restraints on people. This is a key requirement of the Health and Disability Standard for Use of Restraint.
Keep a record
It means that your policy and procedure should ensure that a record is kept of details like:
- when, why and how restraint was used
- the impact and outcome of the restraint
- support and debriefing that was provided or offered to the person
- how the use of the restraint was monitored
- how a recurrence can be prevented in the future.
Report and improve
It also means that your policy and procedure should require reporting. Firstly, as an incident report. Secondly, that aggregate data on restraint incidents are shared at all levels of the organisation so that trends and systemic issues can be identified and addressed.
Lastly, your policy and procedure should support accountability for change and improvement.
If improvements are indicated from review at a client and/or aggregate level of restraint incidents, your policy should require these to be made unless there is good reason not to do so (aka an exceptional reason not to). The decision with reasons should be documented.
There’s a lot to do to prepare for the new Standards. So let us help.
Get in contact to find out more about our online policy and procedure service at the Policy Place.
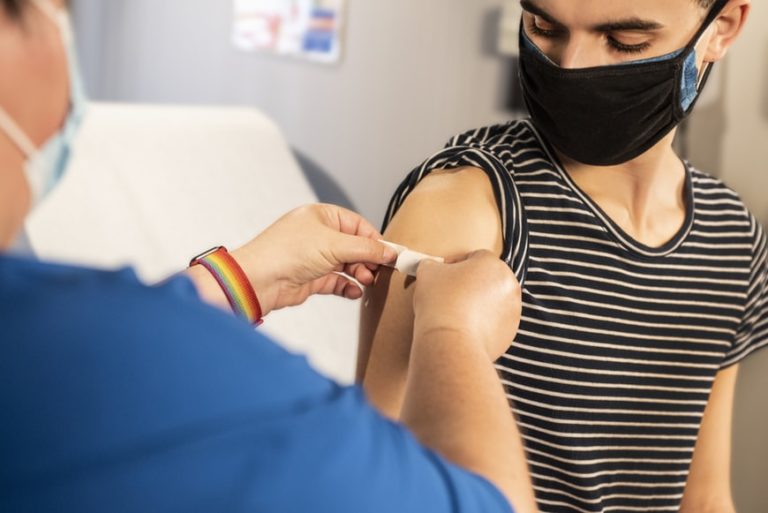
Policies and procedures for vaccination privacy
Privacy policy and procedure is a common accreditation requirement in health and disability, social service and education sectors. At the Policy Place we help people and agencies with their policies and procedures for accreditation purposes. We see Privacy policies in all shapes and sizes.
The best policies and procedures are simple, accessible and usable. They reflect that Privacy law is basically about treating personal information carefully and respectfully.
Some of the worst types of policies are those that are excessively long and make privacy very complex.
Today, we look at policy and procedure implications of some rules of the Privacy Act 2020 as they relate to workplace vaccination requirements. We keep it simple.

Less is best – 3 Privacy Principles
The Information Privacy principles 1, 9 and 10 stiputate requirements for collecting, using, storing and sharing personal information. They are important and relevant to the collection and use of vaccination information from kaimahi/staff.
Privacy Principle 1 requires that only information relevant to purpose should be collected.
Privacy Principle 9 prescribes that personal information should not retained for longer than necessary and Privacy Principle 10, that you can’t use personal data for purposes other than for the reason it was collected.
So … don’t collect more than what is needed; don’t keep or use more than you need; and stick to the initial purpose for collecting the information. If it’s sufficient to sight personal information like vaccination information, then do that. Don’t record or photograph what you don’t need.
Vaccination information for mandated staff
Public health orders mandating vaccinations, require health, disability, education and prison-related services to collect and record vaccination information about kaimahi/staff including details about:
- whether they are in a mandated
- any doses of a COVID-19 vaccine the person has received, or
- the dates by which vaccination must be and was achieved
- whether the person relies on an exemption
- written verification of an exemption if relied on
- other criteria specified in law.
The legislation requires a written record or if it’s digital, for the information to be easily accessible and able to be converted into written form.
Information collection for non-mandated workforce
For other kaimahi whom an organisation decides, after risk assessment, should be vaccinated, there are no legislated requirements about collecting and using vaccination information. Not yet anyway.
For this category, the Information Privacy principles should be applied carefully and cautiously.
Your purpose, when collecting the vaccination/exemption information, is king. Your purpose is to manage risks to the health and safety of your client group and other staff.
It should determine what and why you collect the information and how long you retain it for.
Keep this purpose in mind when deciding how to collect the information. Is it sufficient to sight evidence of full vaccination or is more recording necessary? Be guided by the purpose when deciding what vaccination to collect.

Don’t forget to tell
Information Privacy Principle 11 limits the disclosure of personal information to third parties to when consent is given and a limited range of other situations.
It means that when collecting information about vaccination status, you need to inform staff that you may need to share their information with Ministry of Health, WorkSafe and any other entity that may require your staff to be vaccinated.
On the other hand, if you’re collecting vaccination information from whānau/clients accessing your social, education or health service – then you will need to tell them that the purpose is to mitigate health and safety risks in service delivery. On this basis, different information may be required from a non-vaccinated person and a vaccinated person because the health and safety implications will be different.
Your policies and procedures…
Policy and procedure to guide your approach to collecting and managing vaccination information about kaimahi/staff is crucial at this time. Keep it simple!
At the Policy Place, we have both a Vaccination policy and Privacy policy suite online for our members. Interested in joining us?
Contact us now to talk about your needs.
Mandatory vaccination policies and procedures
It’s all on with mandatory vaccination for social, health, education and prison staff in Aotearoa.
Employing agencies need to move quickly on their vaccination policy and procedure.
The Mandate
The COVID-19 Public Health Response (Vaccinations) Amendment Order (No 3) 2021 has commenced. It provides for mandatory vaccination of certain roles in health, disability, education, and prison services (“mandated roles”).
At the Policy Place, we’ve been busy updating our policies and procedures for our members, because the pressure is on for services that have staff in mandated roles. The legislation sets a fast pace.
Staff in mandated roles in health, disability and education services must receive their first vaccination by 15 November 2021. Staff involved with prisons must receive their first vaccination by 6 November 2021.
In this post, we outline some key responsibilities for employers and staff affected by the new Public Health order.
Management responsibilities
In the new regime, management’s responsibilities will include to:
- Notify staff in writing that their roles are affected by legal requirements. Staff should be told of legal timeframes, consequence of non-compliance and how they may prove vaccination within the timeframes.
- Actively protect rights of tangata whenua and address barriers to vaccination for Māori and Pasifika
- Enable staff (especially those in mandated roles) to be vaccinated in work hours
- Proactively and in good faith engage with staff about any issues or concerns about vaccination
- Being prepared to stand-down staff who are unable to provide written confirmation of vaccination by required dates (eg 15 November for education, health and disability service workers; 6 November for prison staff)
- Set up a system for recording vaccination information from staff (eg contact details, dates of vaccination, exemption from vaccination).
Staff/kaimahi responsibilities
Key responsibilities of staff will include to:
- Get vaccinated within the legal timeframes
- Be informed (by reliable means) about vaccination and the legal requirement
- Engage in good faith with management about any concerns or issues with vaccination (eg if dispute they are in a mandated role)
- Provide management with written proof of vaccination (by registering on My Covid Record and providing a screen-shot or printout of the result)
- If relevant, obtain an exemption from a GP or other suitable health practitioner and provide written confirmation.
What if vaccination is not legally prescribed?
Check out our previous posts on risk assessing roles to decide if vaccination should be required.
Just because a role is not required by law at this stage to be vaccinated, does not prevent an employer from requiring vaccination where they assess high risk.
Every organisation will need to demonstrate due diligence in managing the health and safety of Covid-19 in the workplace and use of vaccination to mitigate risk.
It’s likely to be an ongoing process.
Given the nature of community transmission, risks are likely to change and so are decisions about the necessity of vaccination.
Contact us at the Policy Place if you need a hand with your vaccination policy and procedure.
How to achieve balance in your vaccination policy
Aotearoa has now joined other countries to require health and community support workers and teachers to be vaccinated for Covid-19. At the Policy Place, we’re updating our Vaccination policy and procedure for our members to prepare for the changes.
But what about in other areas of social and community services? Can and should your organisation’s policies and procedures require staff to be vaccinated for Covid-19?
Short answer: it’s a balancing act.
A careful approach
Worksafe has consistently advised that a cautious approach be taken to imposing a vaccination requirement. More recently, it has listed some questions for management and staff to consider when developing their policy on vaccination and considering a requirement for vaccination. Check out the questions here to help you draft your Vaccination policy and procedure.
Risk assessment in your vaccination policy
For social and community services, who are not going to be covered by the Public Health Order requirements for vaccination, your organisation’s policies and procedures should provide for job roles to be assessed for risks of exposure to and transmission of Covid-19.
To assess risks, we suggest you consider the following:
- Public Health and sector/ industry advice on vaccination
- the extent to which the role exposes staff to a risk of exposure to Covid-19
- whether the role involves working with people who are vulnerable to severe disease/death if they are infected
- how many people the role interacts with (could it lead to ‘super-spreading’ event if the person in the role was to contract COVID-19)
- the effectiveness of other infection/ transmission control measures (eg masks; office barriers) at minimising the risk of infection and transmission across staff and those we work with
- other relevant factors (eg rate of community transmission).
Don’t discriminate in your vaccination policy
It’s also important to consider if there are likely to be any discriminatory impacts.
We know that more needs to be done to support tangata whenua, Pasifika and younger people to be vaccinated. A blanket requirement for new and existing staff to be vaccinated could therefore have a discriminatory impact on these groups.
It’s about balancing…..
As we’ve said before, your policy and procedure on vaccination needs to be carefully balanced.
On the one hand, legal responsibilities to protect kaimahi and clients from preventable harm must be fulfilled. On the other hand, your vaccination policy and procedure must avoid discriminatory impacts and give you enough flexibility to work with staff who are unable to be or haven’t yet been vaccinated on options to keep safe in the workplace.
If you’re wanting help with your vaccination policy, contact us – we’ll be 😊 to work with you!
5 takeaways from the Coroner’s and Ombudsman’s children’s reports
The Ombudsman and Coroner reports, released this month, identified inadequate treatment and care of children/tamariki by Crown agencies. The Coroner was reviewing the tragic death of a young two-year-old. The Ombudsman was reviewing policies and practices relating to the removal of newborn babies from their parents and whānau by Oranga Tamariki- the Ministry for Children.
Both reports identified big policy problems that we can all learn from.
Coroner’s report – In the matter of Hineihana Sosefina Mausii

The Coroner was looking into the tragic death of 2-year-old Hineihana Sosefina Mausii in 2013. There had previously been a serious adverse event (SAE) review by the Southern District Health Board(SDHB) and an investigation and review by the Health and Disability Commissioner. Both reviews had found critical failures in Hineihana’s care.
The question for the Coroner was whether she should make any comments or recommendations to reduce the chance of further deaths in similar circumstances.
Key findings of facts
The key facts were that Hineihana was taken twice, within 48 hours, to the Emergency Department(ED) of Dunedin Hospital with an acute health condition. On her second presentation, she was assessed by a junior doctor working under the supervision of a senior doctor. His assessment was found to have been inadequate and to have missed “red flags” about Hineihana’s poor health.
The senior doctor, responsible for supervising the junior doctor, failed to provide an adequate level of supervision appropriate to the junior doctor’s level of experience. As a result, Hineihana’s acute condition was not identified when it should have been. She was wrongly discharged with her parents not given any discharge information about follow up care and when to return to the ED.
Policy gaps
With her preventive hat on, the Coroner identified a couple of big policy gaps that had contributed to Hineihana’s inadequate treatment.
At the time of Hineihana’s re-presentation to the ED there had been no clear policy requiring her (ie as a child) to be assessed by a senior registrar or consultant. The SDHB claimed that requirement had since been introduced. The Coroner however disagreed.
Although it was stated as a requirement in several documents, there was no “single source of truth” aka operational policy requirement for unscheduled representations of children to ED within 48 to be assessed by a senior doctor. The status of the documents mentioning the requirement was unclear. So was the “requirement.” She recommended that this be addressed to prevent future tragedy.
The second policy gap concerned safety-netting at discharge. The SAE Review recommendations included the development of a written policy for safety-netting, and provision of both spoken and written advice for patients/parents/caregivers regarding when to return to the ED. It hadn’t yet been done. The Coroner reinforced the recommendation.

Ombudsman’s Inquiry
The Ombudsman reported back this month on their inquiry into the removal of newborns/pēpi from their parents. It made a number of key findings about poor practice. They also identified some critical policy gaps and errors concerning:
- the use of without notice s78 applications (interim custody applications) and criteria for how staff should identify and assess the viability of other options to make tamariki safe
- working effectively and equitably with disabled parents and other parents suffering from mental distress and drug and alcohol issues (ie using a disability-rights approach)
- for unborn and newborn pēpi, policy requiring:
- trauma-informed social work practice to be applied to assessments of the parents’ own childhood histories of abuse or neglect
- specialist assessments for parents with alcohol or drug misuse, mental health needs or intellectual disabilities.
- the Ministry to assist parents and whānau where their pēpi has been identified as at risk.
- a lack of policy guidance about the process of removing a pēpi from their parents once a s78 interim order has been granted.
The Ombudsman recommended these gaps be addressed to support better decisions and large scale practice change by the Ministry when care and protection are held for newborns.
Key takeaways
Although these reports were looking at different issues. They shared a focus on the care, health and wellbeing of our most precious tamariki. They identified and recommended that some key policy problems be fixed.
Although they concerned Crown agencies, there are some key takeaways for social and health services:
- critical issues that require the application of professional judgement and skill should be supported by operational policy requirements
- policy should reflect legal requirements and in the area of disability and mental health the United Nations Convention on the Rights of People with Disabilities
- to avoid confusion and uncertainty in the workforce, there should be a “single source of truth” when it comes to requirements and this should be your operational policy
- organisational policy must be usable and accessible for busy operational staff
- training should align with and support good operational policy.
If you want to know more about how our online policy and procedure service can support good practice and your compliance with regulations and standards, contact us.
Big push for pastoral care
Parents will be able to rest easier with the Interim Pastoral Care Code now issued for domestic tertiary students.
The Code requires tertiary providers to actively support the social and mental wellbeing of students and to have policies and processes in place to achieve this. Here’s a quick summation of some key provisions.
General obligations
The obligations of tertiary providers include:
- information and advice to students about matters relating to their health and wellbeing
- providing opportunities for students to have experiences that improve their physical or mental health and wellbeing
- staff training on how to recognise and effectively respond to students who may have problems with health or wellbeing
- identifying and assisting students at risk of harm to self and/or others
- assisting disabled students to access appropriate support where required
- helping students prepare for, and adjust to tertiary study
- assisting students and staff to recognise and respond to discrimination, racism, bullying, and harassment (including sexual harassment).
Student accommodation
Student accommodation providers are required to keep watch over and check on the wellbeing of students, monitor risks and have responsive pastoral care practices.
To provide a positive living environment, they must:
- have house rules that promote student safety and wellbeing
- support health promotion activities
- promote responsible social behaviour and academic success
- meet the cultural needs and aspirations of all groups
- develop appropriate initiatives guided by students to build a sense of community.
Right to participate
The right of students to participate in planning and decisions is recognised. Tertiary and accommodation providers must partner with students around support for their learning and pastoral care.
Providers must give students information and advice to help them:
- make positive choices impacting on wellbeing (eg about drug and alcohol use, safe sex)
- use internal complaints processes; and
- make a complaint to the code administrator if a student is dissatisfied with the outcome or experience of using internal complaints processes.
Consent and mandated clients
Informed consent is a human right. But honouring it for clients who are mandated by a court or statutory agency can be a challenge. We look here at how your organisational policy on informed consent can be helpful.
Is this you?
Your organisation has a policy on consent. It has never been an issue because you have always worked with voluntary clients.
But things have changed.
You are now funded to deliver a response to offending, family violence or other problem that used to be dealt with by formal statutory or court intervention. The alternative for the client, as the context for their engagement with you, was a formal or worse intervention (eg conviction, or prison).
What does this mean for your organisational policy on consent?
In these circumstances, consent is undoubtedly compromised. Yet you are required by the Social Services Accreditation Standards and Public Health and Disability Standards to have policy and procedures to ensure all clients (whether mandated or not) exercise their right to informed consent.
So what should your organisation’s policy provide and is there potential for it to help transform an involuntary and unequal situation into more of a voluntary one? YES. A good informed consent policy can help guide empowering practice and authentic engagement with clients. Here’s what we see as some key elements of this type of policy.
Consent is a process
Your policy needs to recognise that there are multiple points in the relationship with a client where consent can be sought. Each of these points offers the client the chance to re-assert their rights to autonomy and make decisions for themselves; to help equalise the situation.
While a person should be asked to consent when they enter a service, this should not be with carte blanche effect. It should only mark the beginning of the consent process. Your policy should require that consent is sought at every key point of involvement with the client. It should be supported and reinforced by other policies addressing client/whānau rights to participate and person/whānau centred responses.
Culture matters
In the Anglo world, certainly in the liberal western tradition of thought, consent is seen in individualistic terms. But that’s just one perspective. Both the significance and process of giving consent can vary cross-culturally and this needs to be recognised in your policy. Important policy requirements include accessing cultural advice and asking the client about their expectations for giving consent. Where collective cultural values are important, the consent process may need to allow for time and the participation of whānau and others.
Be real
Acknowledging the constraints on a client’s choices is important. It’s essential for building an open and honest relationship with a client/whānau. It’s integral to empowering the client within the consent process.
A consent policy should therefore require kōrero with the client about the reasons and conditions of the referral and consequences of non-compliance with those conditions. And don’t forget to cover your agency’s role and responsibilities.
You must explain to the person ordered to attend a Family Violence Perpetrator programme or a young person attending your service as part of their Supervision with Activity order that your agency will have to report to the court/Oranga Tamariki if they don’t comply with the terms of service and likelihood of a court-imposed sanction.
Inform, inform
The Health and Disability and Social Services Accreditation Standards require informed consent. This means providing the full raft of information that a client needs to make their decisions and giving accurate and balanced information. Options should be canvassed and the consequences of giving or refusing consent (e.g risks, benefits, costs). The client should be encouraged to ask questions on the basis there are no silly questions
We all need support
The last but probably one of the most important policy requirements is that we should assume a client will need support to give consent. We work with clients often in mental distress or dealing with conditions or circumstances that can diminish their capacity to make decisions and give informed consent.
We should assume support will be needed unless there are grounds to show otherwise. What the support involves will depend on the client. It could range from whānau, communicative assistance, use of an Easy Read translation or linking a person to an advocate eg Health and disability advocate, Disability organisation, VOYCE for a young person in care or legal guardian.
Conclusion
We can’t avoid or shy away from the reality that we are often working with clients in coercive contexts. But there are still many opportunities for a client to exercise choice about engaging with your service.
Yes, engagement is about manaakitanga and skilled work. It’s also about respecting and supporting a person to make their own decisions and give or not give consent in an informed way.
Your Informed Consent policy is important not just to comply with accreditation standards but because it supports client empowerment and authentic and transformative relationships with clients.
Q and A Family violence information sharing
Changes to support information sharing about family violence are due to commence on 1 July 2019. Here’s some Q&As about what’s coming.
Q-Why is information-sharing being changed?
answer
Death reviews have shown missed opportunities to respond to family violence. The new information-sharing provisions aim to address this.
Q-Who’s affected?
answer
The new law applies to family violence agencies and social services practitioners. Both are defined broadly. Community services receiving government funding to help victims and/or to stop perpetrators of family violence, licensed early childhood services, schools and specified government agencies are included.
Q-What’s the change?
answer
There are some legal requirements. The gist of the changes is that if you’ve got information that could help another agency working with a person impacted by family violence then consider sharing it. It’s not compulsory to share the information but it is compulsory to consider sharing it.
This is important particularly for people working in health-related agencies who often feel conflicted about their duty of confidentiality versus sharing information.
Q–What happens if I share info?
answer
As long as you share information in good faith and are careful you wont be liable. You should check the relevance of the personal information requested or that you’re thinking about disclosing (eg is it relevant to a client’s assessment or plan?)
Q–What if a client doesn’t want to share their info?
answer
The point of the change is that safety rather than consent should drive information sharing.
Best efforts should be made to obtain a person’s consent to sharing their personal information and you should consider their views. But even if consent is withheld, you might decide the information should be shared eg to help with safety planning.
Q–What about a client’s trust?
answer
This is often a big worry. People trust us with information and we want to honour that trust. But the new law means we don’t have to put this above protecting a victim from violence.
We can still build and maintain trust. But it needs to be done from the start. Clients should be informed when welcomed to the service that personal information may be shared if it will help protect a victim of family violence. Transparency should then be maintained throughout the relationship when and if their personal information is shared for family violence reasons.
Q–What does it mean for policies?
answer
We’ve been updating our online policy service for members. Policies that are being updated include those dealing with privacy and planning.
We’ve had a lot of people join us lately, but it’s still a good time to join.
It takes about 8 weeks to get you online. But we’ll put you online with your policies updated. From then on, we regularly review them and keep them up-to-date.
Contact us if you need a hand.